| Skin Cancer
Basic Information
The two most common types of skin
cancer-basal cell and squamous cell carcinomas-are
highly curable. However, melanoma, the third most
common skin cancer, is more dangerous, especially
among young people. Approximately, 65%-90% of melanomas
are caused by exposure to ultraviolet (UV) light or
sunlight.
1. Basal Cell Carcinoma
What Is Basal Cell Carcinoma?
Basal cell carcinoma (BCC) is the
most common form of cancer. Basal cells line the deepest
layer of the epidermis. Basal cell carcinomas are
malignant growths--tumors--that arise in this layer.
Basal cell carcinoma can usually
be diagnosed with a simple biopsy and is fairly easy
to treat when detected early. However, 5 to 10 percent
of BCCs can be resistant to treatment or locally aggressive,
damaging the skin around them, and sometimes invading
bone and cartilage. When not treated quickly, they
can be difficult to eliminate. Fortunately, however,
this is a cancer that has an extremely low rate of
metastasis, and although it can result in scars and
disfigurement, it is not usually life threatening.
Cause
The sun is responsible for over
90 percent of all skin cancers, including BCCs, which
occur most frequently on the sun-exposed areas of
the body: face, ears, neck, scalp, shoulders, hands and feet.
Am I At Risk?
Anyone with a history of frequent
or intermittently intense sun exposure can develop
BCC, but a number of factors increase risk:
Time Spent Outdoors People who work outdoors - construction
workers, groundskeepers, lifeguards, etc. - are at
greater risk than people who work indoors, as are
those who spend their leisure hours in the sun.
Skin Type Fair-skinned individuals who sunburn easily
and tan minimally or not at all have a higher incidence
of skin cancer than dark-skinned individuals. Check
our skin type chart to see how at risk you are.
Hours of sunlight the more hours of sunlight in the
day, the greater the incidence of skin cancer.
Warning Signs
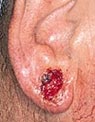 The
five most typical characteristics of basal cell carcinoma
are shown in the pictures below. Frequently, two or
more features are present in one tumor. In addition,
BCC sometimes resembles non cancerous skin conditions
such as psoriasis or eczema. Only a trained physician
can decide for sure. If you observe any of the warning
signs or some other change in your skin, consult your
physician immediately. The
five most typical characteristics of basal cell carcinoma
are shown in the pictures below. Frequently, two or
more features are present in one tumor. In addition,
BCC sometimes resembles non cancerous skin conditions
such as psoriasis or eczema. Only a trained physician
can decide for sure. If you observe any of the warning
signs or some other change in your skin, consult your
physician immediately.
 An
Open Sore that bleeds, oozes or crusts and remains
open for a few weeks. A persistent, non-healing sore
is a very common sign of an early basal cell carcinoma. An
Open Sore that bleeds, oozes or crusts and remains
open for a few weeks. A persistent, non-healing sore
is a very common sign of an early basal cell carcinoma.
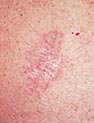
 A
Reddish Patch or irritated area, frequently occurring
on the chest, shoulders, arms or legs. Sometimes the
patch crusts. It may also itch or hurt. At other times,
it persists with no noticeable discomfort. A
Reddish Patch or irritated area, frequently occurring
on the chest, shoulders, arms or legs. Sometimes the
patch crusts. It may also itch or hurt. At other times,
it persists with no noticeable discomfort.
 A
Shiny Bump or nodule that is pearly or translucent
and is often pink, red or white. The bump can also
be tan, black or brown, especially in dark-haired
people, and can be confused with a mole. A
Shiny Bump or nodule that is pearly or translucent
and is often pink, red or white. The bump can also
be tan, black or brown, especially in dark-haired
people, and can be confused with a mole.
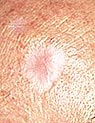 A
Pink Growth with a slightly elevated rolled border
and a crusted indentation in the center. As the growth
slowly enlarges, tiny blood vessels may develop on
the surface. A
Pink Growth with a slightly elevated rolled border
and a crusted indentation in the center. As the growth
slowly enlarges, tiny blood vessels may develop on
the surface.
A Scar-Like Area which is white, yellow or waxy, and
often has poorly defined borders. The skin itself
appears shiny and taut. This warning sign can indicate
the presence of small roots, which make the tumor
larger than it appears on the surface.
2.Squamous Cell Carcinoma
What Is Squamous Cell Carcinoma?
Squamous cell carcinoma (SCC) is
the second most common form of skin cancer, with over
250,000 new cases per year estimated in the United
States. It arises in the squamous cells that compose
most of the upper layer of the skin.
Most SCCs are not serious. When
identified early and treated promptly, the future
is bright. However, if overlooked, they are harder
to treat and can cause disfigurement. While 96 to
97 percent of SCCs are localized, the small percentage
of remaining cases can spread to distant organs and
become life-threatening.
Cause
Most cases of squamous cell carcinoma
are caused by chronic overexposure to the sun. Tumors
appear most frequently on the sun-exposed face, neck,
bald scalp, hands, shoulders, arms and back. The rim
of the ear and the lower lip are especially vulnerable
to these cancers.
SCCs may also occur where skin has
suffered certain kinds of injury: burns, scars, long-standing
sores, sites previously exposed to X-rays or certain
chemicals (such as arsenic and petroleum by-products).
In addition, chronic skin inflammation or medical
conditions that suppress the immune system over an
extended period of time may encourage development
of the disease.
Occasionally, squamous cell carcinoma
arises spontaneously on what appears to be normal,
healthy, undamaged skin. Some researchers believe
that a tendency to develop this cancer may be inherited.
Am I at Risk?
Anyone with a substantial history
of sun exposure can develop squamous cell carcinoma
but certain environmental and genetic factors can
increase the potential for this disease. Sun Exposure:Sunlight
is responsible for over 90 percent of all skin cancers.
Working primarily outdoors, living in an area that
gets a lot of high intensity sunlight (like Australia),
and spending time in tanning booths all increase your
exposure to UV rays and thus increase your risk for
developing skin cancer, including squamous cell carcinoma.
Skin Type : People
who have fair skin, light hair, and blue, green, or
gray eyes are at highest risk. Hispanics, Asians and
dark-skinned individuals of African descent are far
less likely than Caucasians to develop skin cancer.
Check out your skin type and how it affects your skin
cancer risk.
More than two thirds of the skin
cancers that dark-skinned individuals develop are
SCCs, usually arising on the sites of preexisting
inflammatory skin conditions or burn injuries. It
is still essential for them to practice sun protection.
Previous Skin Cancer :
Anyone who has had a skin cancer of any type is at
increased risk of developing another one.
Reduced Immunity :
People with weakened immune systems due to excessive
unprotected sun exposure, chemotherapy, or illnesses
such as HIV/AIDS are more likely to develop squamous
cell carcinoma.
What to Look For
Squamous cell tumors are thick,
rough, horny and shallow when they develop. Occasionally,
they will ulcerate, which means that the epidermis
above the cancer is not intact. There will be a raised
border and a crusted surface over a raised, pebbly,
granular base. See photos below for examples.
Any bump or open sore in areas of
chronic inflammatory skin lesions indicates the possibility
of squamous cell carcinoma, and a doctor should be
consulted immediately if this is the case. Usually,
the skin in these areas reveals telltale signs of
sun damage, such as wrinkling, changes in pigmentation
and loss of elasticity. That is why tumors appear
most frequently on sun-exposed parts of the body.
Precancers and Early Cancers
There are some precursor conditions,
called precancers and early cancers (also called carcinoma
in situ) that are sometimes associated with the later
development of SCC. They include actinic keratosis,
actinic chelitis, leukoplakia, and Bowen's disease,
although most dermatologists believe that Bowen's
disease is just another name for a type of superficial
SCC that hasn't spread yet. It appears as a persistent,
scaly red-brown, scaly patch. It may resemble eczema
or psoriasis.
If you notice any change on your
skin - a mole changing appearance, a new growth, a
sore that won't heal - have a doctor look at it without
delay. Treatments for early cancers are much more
effective than treatments for later ones.
Warning Signs
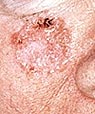
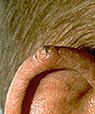 A
wart-like growth that crusts and occasionally bleeds A
wart-like growth that crusts and occasionally bleeds
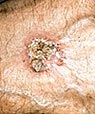
 A
persistent, scaly red patch with irregular borders
that sometimes crusts or bleeds. A
persistent, scaly red patch with irregular borders
that sometimes crusts or bleeds.
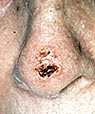
 open
sore that bleeds and crusts and persists for weeks. open
sore that bleeds and crusts and persists for weeks.
 An
elevated growth with a central depression that occasionally
bleeds. A growth of this type may rapidly increase
in size. An
elevated growth with a central depression that occasionally
bleeds. A growth of this type may rapidly increase
in size.
3. Melanoma
What Is Melanoma?
Melanoma is the most serious form
of skin cancer. However, if it is recognized and treated
early, it is nearly 100 percent curable. But if it
is not, the cancer can advance and spread to other
parts of the body, where it becomes hard to treat
and can be fatal. While it is not the most common
of the skin cancers, it causes the most deaths.
Melanoma is a malignant tumor that
originates in melanocytes, the cells which produce
the pigment melanin that colors our skin, hair, and
eyes. The majority of melanomas are black or brown.
However, some melanomas are skin-colored, pink, red,
purple, blue or white.
Am I at Risk?
Everyone is at some risk for melanoma,
but increased risk depends on several factors: sun
exposure, number of moles on the skin, skin type and
family history (genetics).
Sun exposureBoth
UVA and UVB rays are dangerous to the skin,
and can induce skin cancer, including melanoma. Blistering
sunburns in early childhood increase risk, but cumulative
exposure also is a factor. People who live in locations
that get more sunlight - like Florida, Hawaii, and
Australia - get more skin cancer. Avoid using a tanning
booth or tanning bed, since it increases your exposure
to UV rays, increasing your risk of developing melanoma
and other skin cancers.
Moles: There are
two kinds of moles: normal moles - the small brown
blemishes, growths, or "beauty marks" that
appear in the first few decades of life in almost
everyone - and atypical moles, also known as dysplastic
nevi. Regardless of type, the more moles you have,
the greater your risk for melanoma.
Skin Type As with
all skin cancers, people with fairer skin are at increased
risk. You can read more about skin type and risk here.
Family History
About one in every ten patients diagnosed with the
disease has a family member with a history of melanoma.
If your mother, father, siblings or children have
had a melanoma, you are in a melanoma-prone family.
Each person with a first-degree relative diagnosed
with melanoma has a 50 percent greater chance of developing
the disease than people who do not have a family history.
If the cancer occurred in a grandmother, grandfather,
aunt, uncle, niece or nephew, there is still an increase
in risk, although it is not as great. Read more on
family history, below.
Personal History
Once you have had melanoma, you run an increased chance
of recurrence. Also, people who have or had basal
cell carcinoma and squamous cell carcinoma are at
increased risk for developing melanoma.
Weakened Immune System Compromised
immune systems as the result of chemotherapy, an organ
transplant, excessive sun exposure, and diseases such
as HIV/AIDS or lymphoma can increase your risk of
melanoma.
More about Family History
We are all at risk for melanoma.
However, some people are more at risk than others.
Heredity plays a major role. If your mother, father,
siblings, or children (first-degree relatives) have
had a melanoma, you are part of a melanoma-prone family.
Each person with a first-degree relative diagnosed
with melanoma has a 50 percent greater chance of developing
the disease than members of the general public who
do not have a family history of the disease. If the
cancer occurred in a grandmother, grandfather, aunt,
uncle, niece, or nephew (second-degree relatives),
there is still an increase in risk compared to the
general population, though it is not as great.
About one of every ten patients
diagnosed with the disease has a family member with
a history of melanoma. If melanoma is present in your
family, you can protect yourself and your children
by being particularly vigilant in watching for the
early warning signs and finding the cancer when it
is easiest to treat.
Close Relatives Examined
When this skin cancer is diagnosed,
it is standard practice for physicians to recommend
that close relatives be examined immediately for melanoma
and for the presence of unusual or atypical moles.
These moles are also called "dysplastic nevi."
You can read more about atypical moles here.
Family Syndrome
When atypical moles are found in
an individual belonging to a melanoma family, the
condition is known as FAMMM, standing for Familial
Atypical Multiple Mole Melanoma Syndrome. People with
this syndrome are at the greatest risk of developing
melanoma. In contrast, a research study found that
those family members who did not have atypical moles
were much less likely to develop melanoma.
Genetic Risk Factors
A mutation (alteration) in a recently
discovered gene, the BRAF, may play a part in causing
melanoma. In one study, this mutated gene was found
in two-thirds of the melanoma cells analyzed. BRAF
is called a "switch" gene, because it turns
on to allow the cells to grow and divide. Mutations
in this gene can lead to uncontrolled cell growth
and cancer. The discovery is an exciting research
breakthrough, but physicians and patients are still
years away from reaping the rewards. Ultimately, the
understanding of the BRAF gene could lead to the development
of diagnostic tools and drug therapies. The mutations
most commonly seen in familial melanoma occur in another
gene, p53. When this gene is in its normal state,
its main function is to give damaged cells time to
repair themselves and not progress to cancer. However,
when the gene is altered, it becomes unable to perform
this function, and cancer can result. A number of
gene mutations in addition to p53 and BRAF have been
associated with familial melanoma. In the future,
families might be screened so as to identify those
members who are carrying a defective gene.
Moles in an Active Stage
Moles in people belonging to melanoma-prone
families are subject to change at certain times of
life. They may get larger or show alterations in color
or elevation, so for those periods, they are described
as being active. While the reasons for these changes
are not fully known, there could be a hormonal component:
Moles are more active at puberty and during pregnancy.
Many - but not all - physicians advise high-risk individuals
not to take hormonal medications, such as oral contraceptives
or hormone replacement therapy.
Examination Scheduling
Individuals with the Atypical Mole
Syndrome can improve their chances of early detection
by increasing the frequency of skin self-examination
and by visiting a physician more often. The clinician
may take photographs to document whether there are
new moles or changes in older ones.
Children: A Special Case
Children in melanoma-prone families
need special care, because familial melanoma is likely
to make its appearance early in life. Even though
these cancers usually do not appear until after adolescence,
they may arise in much younger children who have a
family history of melanoma. Most physicians, therefore,
advise parents to make a point of studying a child's
skin frequently from infancy on.
Physician examination should start
at the age of ten and continue on a twice-a-year basis
thereafter. Particular care should be taken at puberty
and during adolescence when hormonal changes activate
the moles. Here is some encouraging news: Because
melanoma families are on the lookout for the disease
and seek professional consultation early, the survival
rate for familial melanoma is even higher than that
for non-familial melanomas.
Warning Signs: The ABCDEs of Melanoma
Moles, brown spots and growths on
the skin are usually harmless - but not always. Anyone
who has more than 100 moles is at greater risk for
melanoma. The first signs can appear in one or more
atypical moles. That's why it's so important to get
to know your skin very well and to recognize any changes
in the moles on your body. Look for the ABCDEs of
melanoma, and if you see one or more, make an appointment
with a physician immediately.
Asymmetry
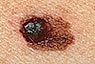 If
you draw a line through this mole, the two halves
will not match. If
you draw a line through this mole, the two halves
will not match.
Border
 The
borders of an early melanoma tend to be uneven. The
edges may be scalloped or notched. The
borders of an early melanoma tend to be uneven. The
edges may be scalloped or notched.
Color
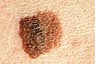 Having
a variety of colors is another warning signal. A number
of different shades of brown, tan or black could appear.
A melanoma may also become red, blue or some other
color. Having
a variety of colors is another warning signal. A number
of different shades of brown, tan or black could appear.
A melanoma may also become red, blue or some other
color.
Diameter
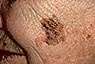 Melanomas
usually are larger in diameter than the size of the
eraser on your pencil (1/4 inch or 6 mm), but they
may sometimes be smaller when first detected. Melanomas
usually are larger in diameter than the size of the
eraser on your pencil (1/4 inch or 6 mm), but they
may sometimes be smaller when first detected.
Evolving
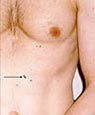 Any
change - in size, shape, color, elevation, or another
trait, or any new symptom such as bleeding, itching
or crusting - points to danger. Any
change - in size, shape, color, elevation, or another
trait, or any new symptom such as bleeding, itching
or crusting - points to danger.
Prompt action is your best protection.
|